Teaching Hospital–Based Medical Education Quality Framework
Learn–Assess–Improve–Govern
What it is: A lightweight but rigorous structure that helps teaching hospitals and universities build a measurable medical education system—without over-engineering.
Where it fits: Designed for teaching hospitals and health sciences universities — including Medicine, Dentistry, and Dental Public Health — where clinical training, community placements, prevention programs, and population health initiatives require structured supervision, measurable assessment, continuous improvement, and accountable governance.
Why this framework exists
Common problems this addresses:
“We teach well” but outcomes and progression are unclear
Assessment varies by assessor and department
Feedback exists but does not drive improvement actions
Governance is ad-hoc; decisions are not data-driven
The four pillars
These four pillars connect learning to reliable assessment, continuous improvement, and leadership governance.
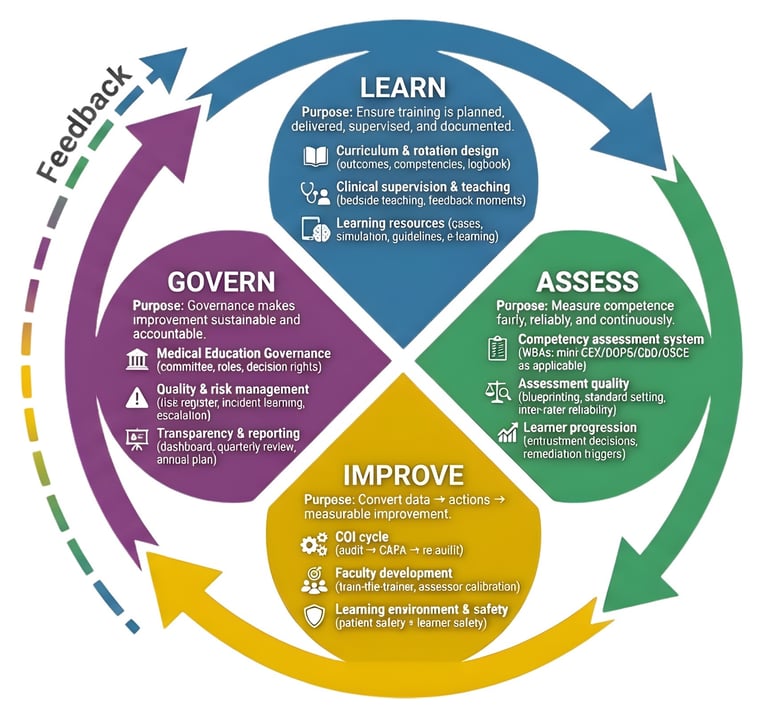
LEARN
Curriculum & rotation design (outcomes, competencies, logbook)
Clinical supervision & teaching (bedside teaching, feedback moments)
Learning resources (cases, simulation, guidelines, e-learning)
ASSESS
Competency assessment system (WBAs and OSCE as applicable)
Assessment quality (blueprinting, standard setting, inter-rater reliability)
Learner progression (entrustment decisions, remediation triggers)
IMPROVE
CQI cycle (audit → CAPA → re-audit)
Faculty development (train-the-trainer, assessor calibration)
Learning environment & safety (patient safety + learner safety)
GOVERN
Medical Education Governance (committee, roles, decision rights)
Quality & risk management (risk register, incident learning, escalation)
Transparency & reporting (dashboard, quarterly review, annual plan)
KPI starter set (example list)
Starter KPIs (customizable)
% rotations with defined outcomes + logbook requirements (target ≥ 90%)
Supervision ratio compliance (e.g., % shifts meeting supervision standard)
Faculty teaching engagement (% faculty meeting minimum sessions)
WBA completion rate per trainee per month (minimum threshold defined locally)
Assessor calibration coverage (% assessors calibrated/6 months)
Assessment reliability signal (e.g., moderation concordance %)
CAPA closure on time (% actions closed by due date)
Re-audit pass rate (% issues improved after 60–90 days)
Remediation success rate (% learners improved after support plan)
Quarterly Medical Education Quality Review held (Y/N + attendance rate)
Learner experience score (pulse survey, response rate + score)
Patient safety learning integration (# cases/M&M linked to learning objectives)
Optional Extension KPIs: Community / Dental Public Health (add-on)
% community/outreach sites meeting minimum training criteria (target ≥ 90%)
Prevention pathway adherence rate (target defined locally)
Follow-up/referral completion rate after screening (target defined locally)
Education delivery rate (% eligible encounters documented) (target ≥ 85% or local)
Underserved reach indicator (target defined locally)
Outreach IPC & safety compliance (target ≥ 95% or local)
Adoption pathway (90 days)
90-day adoption (high-level)
Weeks 1–2: baseline scan + gap map
Weeks 3–4: KPI definitions + dashboard skeleton
Weeks 5–8: pilot in 1–2 departments
Weeks 9–12: governance cadence + scale plan
Contact
Building measurable, internationally-aligned medical education quality systems for teaching hospitals, health sciences universities, and dental/community-based programs.
info@medical-edu.com
© 2026. All rights reserved.
